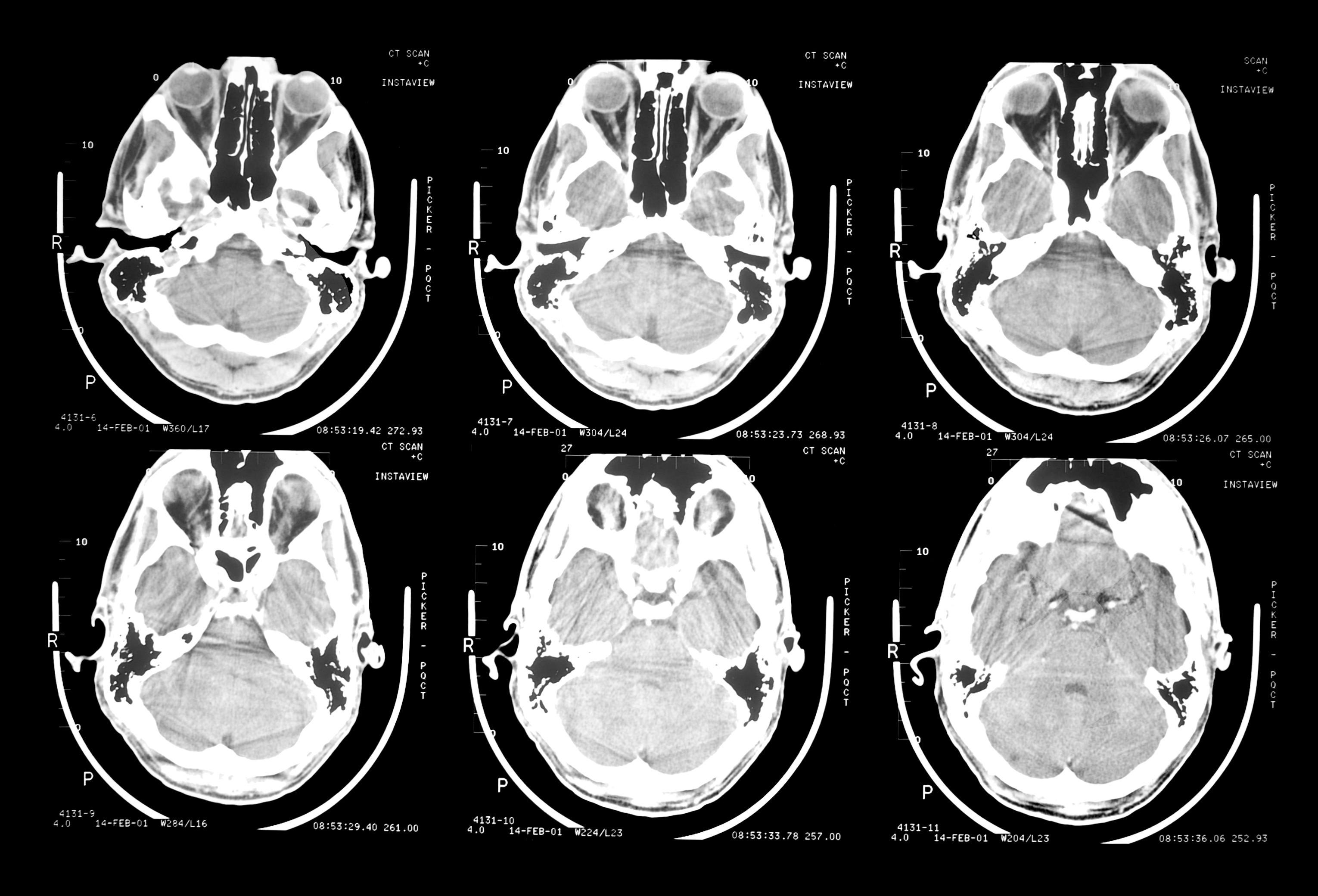
PET Scans Show Brain Degeneration in Living NFL Football Players
In the February 2013 issue of the American Journal of Geriatric Psychiatry, Dr. Gary Smalls and colleagues published research on their use of PET scans to search for abnormal deposits of tau protein in the brains of living people. Excessive tau has been correlated medically with such degenerative brain conditions as Alzheimer’s disease