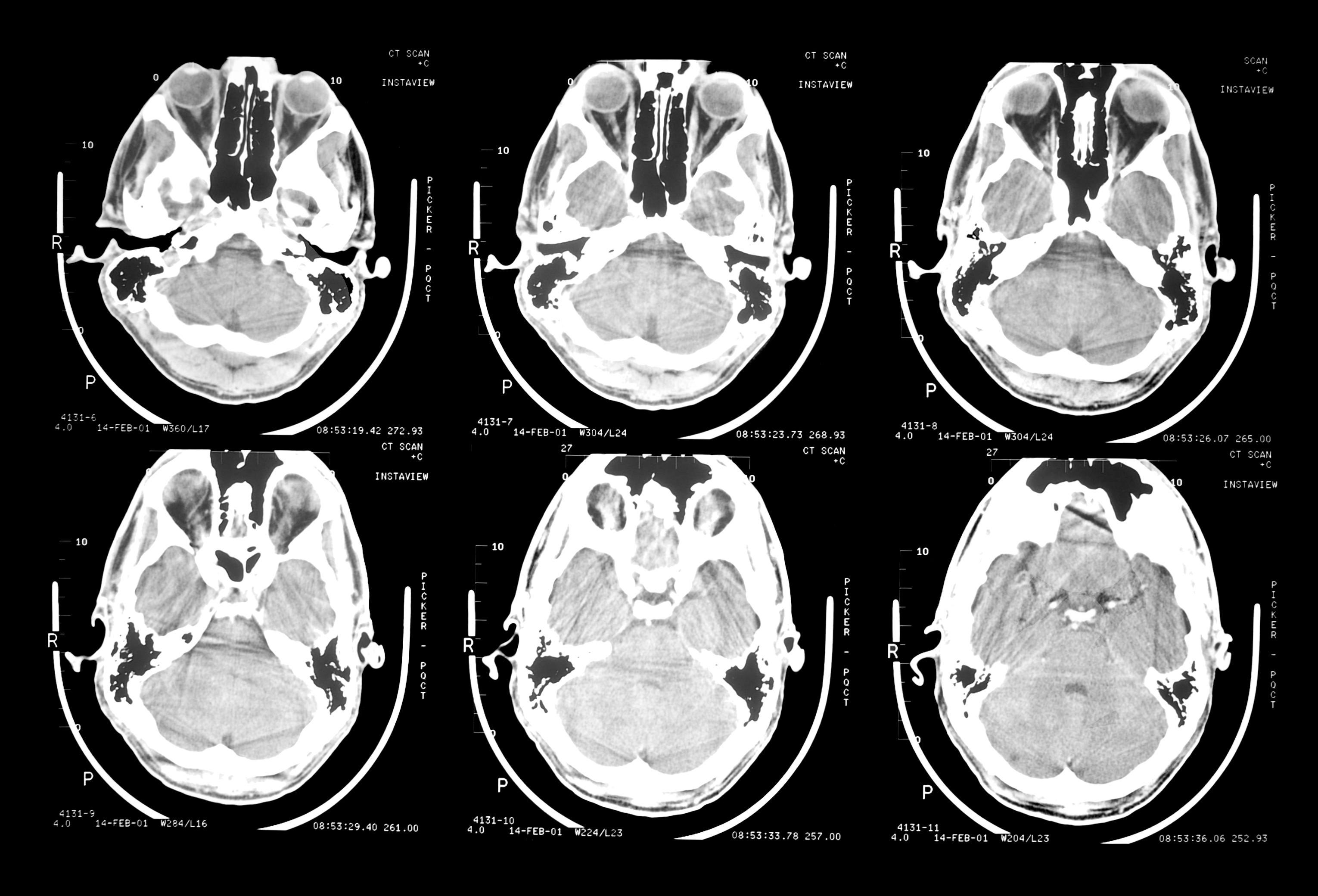
Communication by Brain Waves Alone
Some victims of severe traumatic brain injury are unable to speak at all or speak unintelligibly. What if it were possible for them to wear a set of EEG headphones that recorded their internal thoughts in the form of EEG waves and transmitted their EEG waves via computer to another person? What if