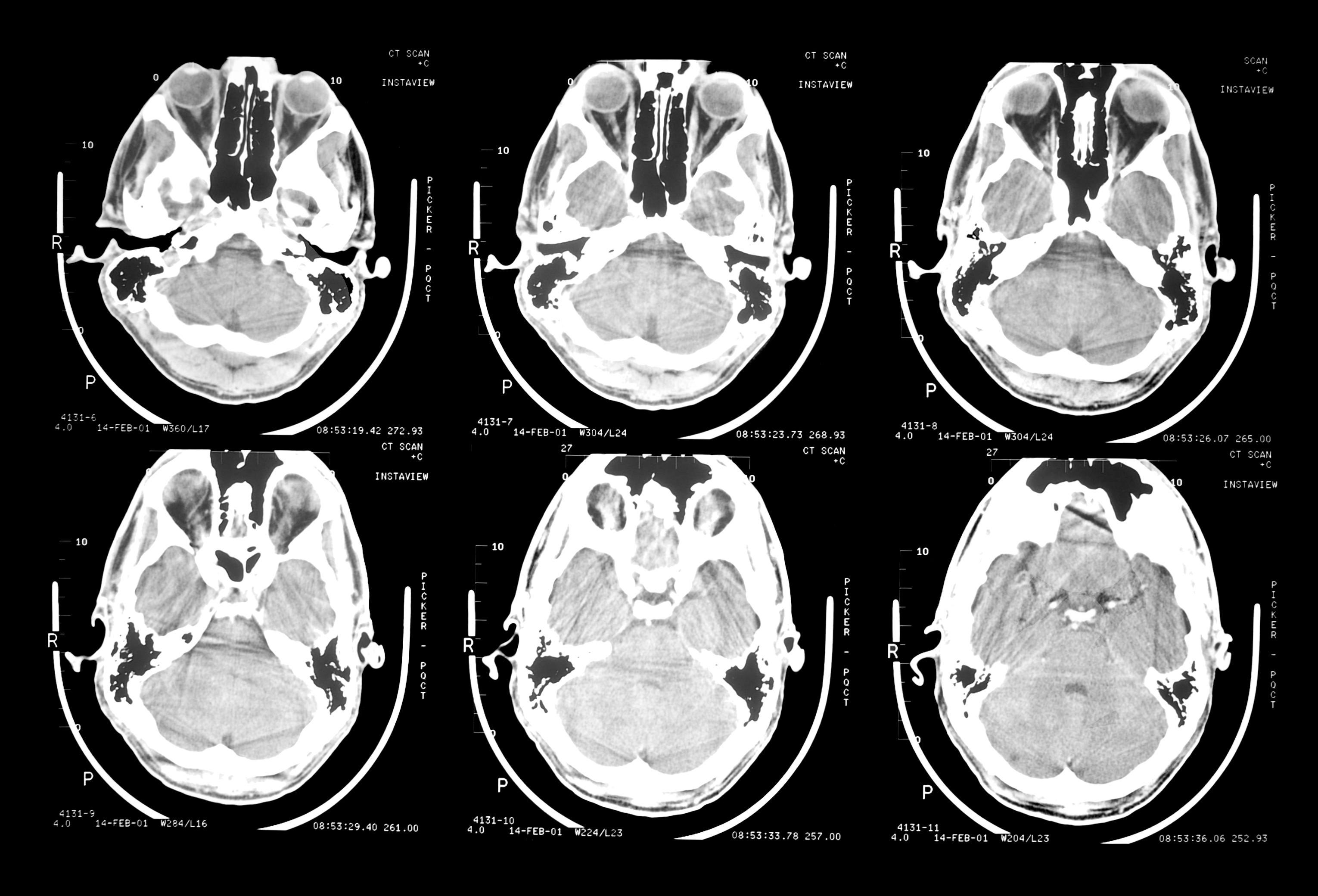
TBI is Consequential. It Causes Homelessness.
Dr. Jane Topolovec-Vranic, a clinical researcher in neuroscience at St. Michael’s Hospital in Toronto, announced that nearly half of the 111 homeless men she studied had suffered at least one traumatic brain injury, and that 87% of them had their brain injury before becoming homeless. The study was published in Open (a journal